Quality by Design in Decentralized Clinical Trials: What is the Role of Technology?

On April 19, the International Conference on Harmonization (ICH) made available an explanatory note and draft version of its updated principles for good clinical practice (GCP). While the principles are considered a “work-in-progress,” they offer an opportunity to reflect on the current vision of the working group and align with the modernized ICH E8 Revision 1 (R1), Revision of General Considerations for Clinical Studies.
When ICH releases ICH E6 (R3) in the fall, it will be composed of an overarching principles document (the draft version noted above) in addition to Annex 1 (addressing interventional clinical trials), and Annex 2 (providing any needed additional considerations for non-traditional interventional clinical trials). The overarching principles document and Annex 1 will replace the current ICH E6 (R2).
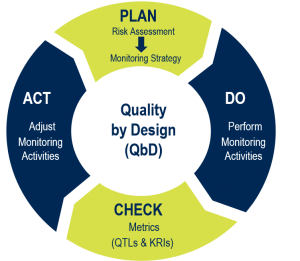
When reflecting on the early draft, one of the most significant messages is the alignment with ICH E8 (R1) in relation to Quality by Design principles. R3 makes it clear that clinical trials set out to ensure that the quality of a trial is driven proactively by designing quality into the study protocol and processes. These activities should be applied during the early planning stages and across trial operations. As the industry witnessed during the COVID-19 pandemic, nearly every global regulatory body which released COVID-19–specific guidance noted the importance of performing risk assessment activities. This reference within R3 fully aligns with R2 regarding the establishment of a culture of quality within organizations.
In addition to the strong emphasis on Quality by Design, there is the introduction of technology to R3 into the principles to support an improved and more efficient approach to trial design and conduct. Within R2, the term technology was used only once, while within the principles document, it’s referenced nine times. This change reflects the modernization of clinical trial operations. The impact of technology on clinical trial operations has been tremendous, and some of the best examples are within the development of COVID-19 vaccines using decentralized trial strategies. Without the contribution of technology, patient participation in clinical trials and oversight activities outside the clinical investigative site would not have been possible. The speed with which these therapies reached the market relied on remote data capture linked to real-time data insights that enabled fast decision-making and issue resolution clearly aligned with the principles of R3.
When technology is applied to clinical trial conduct, it must be adapted to fit individual patient characteristics and the particular trial design. This highlights the core interaction between the application of technology with Quality by Design principles. It comes as no surprise that the best way to address this interaction is with the conduct of a risk assessment during the protocol design phases and throughout trial operations.
Also of note is that R3 transitioned from the use of the term subject to patient. Within R3, the term patient is used 33 times while it was not used in R1 or R2, which highlights the greater emphasis on patient centricity within GCP.
This early draft and explanatory note have been welcome in providing insight into the principles of the new revision, and help to clearly define the role of Quality by Design principles and sound technology deployment in the design and execution of clinical trials.
Watch our webcast, Preparing for ICH E6 (R3) Good Clinical Practice Changes, to understand more about the changes to ICH E6 (R3).
About the Author:
Brian Barnes, Senior Director of Product Management, Clinical Operations Technology, Medidata

Brian Barnes is a Sr. Director, Product Development of RBQM for Medidata Solutions. Brian has 15 years of experience in the clinical development space and has been specifically supporting RBQM for the past nine years, specializing in operational solutions for small to large pharma, biopharma, and biotech companies. Brian is a co-liaison within the Association of Clinical Research Organizations (ACRO) RBQM Working Group and has presented on the topic of RBQM at industry meetings and conferences, and published in journals.
Contact Us
